Diabetes UK
Published on Sep 3, 2013
Related Health Conditions and Vision Complications
1.Nerve pain. Nerve pain caused by diabetes, known as diabetic peripheral neuropathy, can be severe, constant, and hard to treat. Controlling your blood sugar can make a big difference (WebMD, 2018).
2. Heart. Years of high blood sugar may harm your body’s blood vessels. That raises your chance of having heart disease, which can cause heart attacks or strokes later on. High blood pressure and high cholesterol make the problems even more likely (Pathak, 2018).
3. Kidneys. Diabetes can affect blood vessels in your kidneys, too, so they may not work as well. After many years of trouble, they might stop working (Pathak, 2018).
4. Feet. High blood sugar can harm blood flow and damage nerves, and that may cause cuts, scrapes, or sores to heal slowly. You may lose some feeling in your feet, which keeps you from noticing injuries that can get infected. If an infection gets serious, it might mean you need to have a foot removed (Pathak, 2018).
5. Skin. Diabetes may make you more likely to have yeast infections, itching, or brown or scaly patches (Pathak, N., 2018).
6. Erection problems. Men with diabetes may be at risk for sexual problems, because high blood sugar can harm blood flow and damage nerves that the body needs to get and keep an erection (Pathak, 2018).
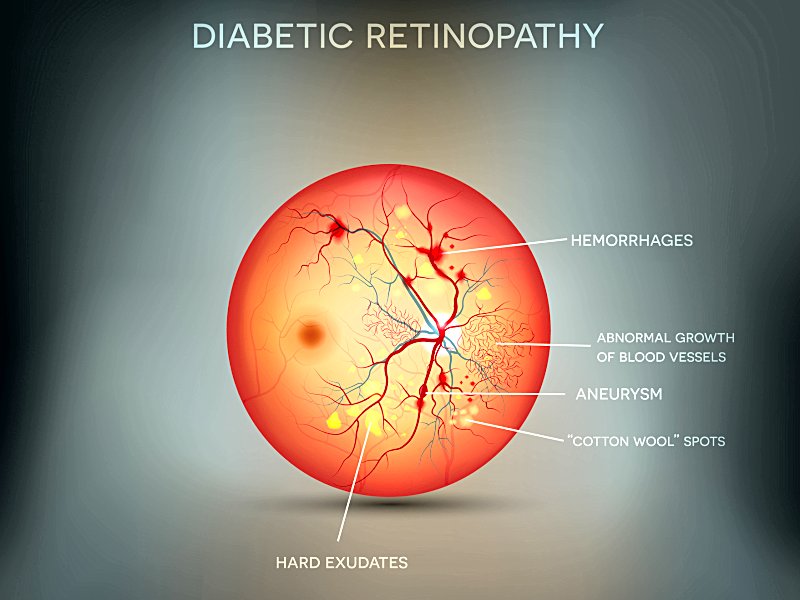
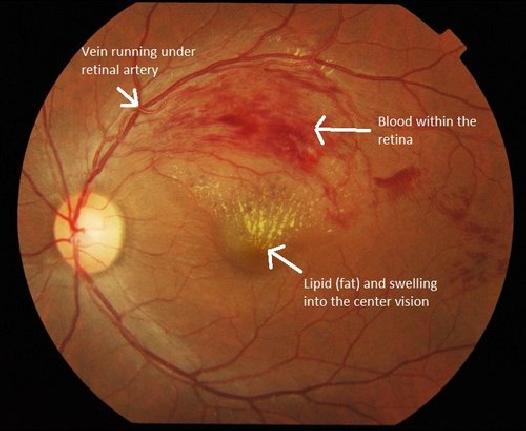
7. Eye problems. Diabetes can increase your risk of eye problems. When your body doesn’t make enough insulin or is unable to use it properly, glucose can build up in your blood and harm your nerves and blood vessels, as shown in the video above. Damage in your eyes from high blood sugar levels can lead to vision problems and blindness. This can happen to anyone with diabetes.
Diabetic Retinopathy
Your eye doctor will use a special dye to look for leaking blood vessels. Leaking blood vessels can cause swelling in your retina (where images focus inside the back of your eye) and decrease your vision. Poor circulation can cause new, weak blood vessels to grow in the retina. These are very prone to bleeding, which can also lead to loss of vision as well as retinal detachment (Kozarsky, A., 2018).
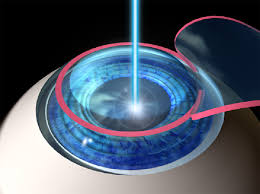
Optional Treatment: Laser Surgery
In the early stages of diabetic retinopathy, your doctor may do a procedure called pan retinal photocoagulation with a laser to destroy large areas of your retina where the abnormal blood vessels grow. It seals the blood vessels and stops them from leaking and growing. This kind of surgery won’t bring your vision back, but with follow-up care, you can lower your chance of blindness by as much as 90% (Kozarsky, A., 2018).
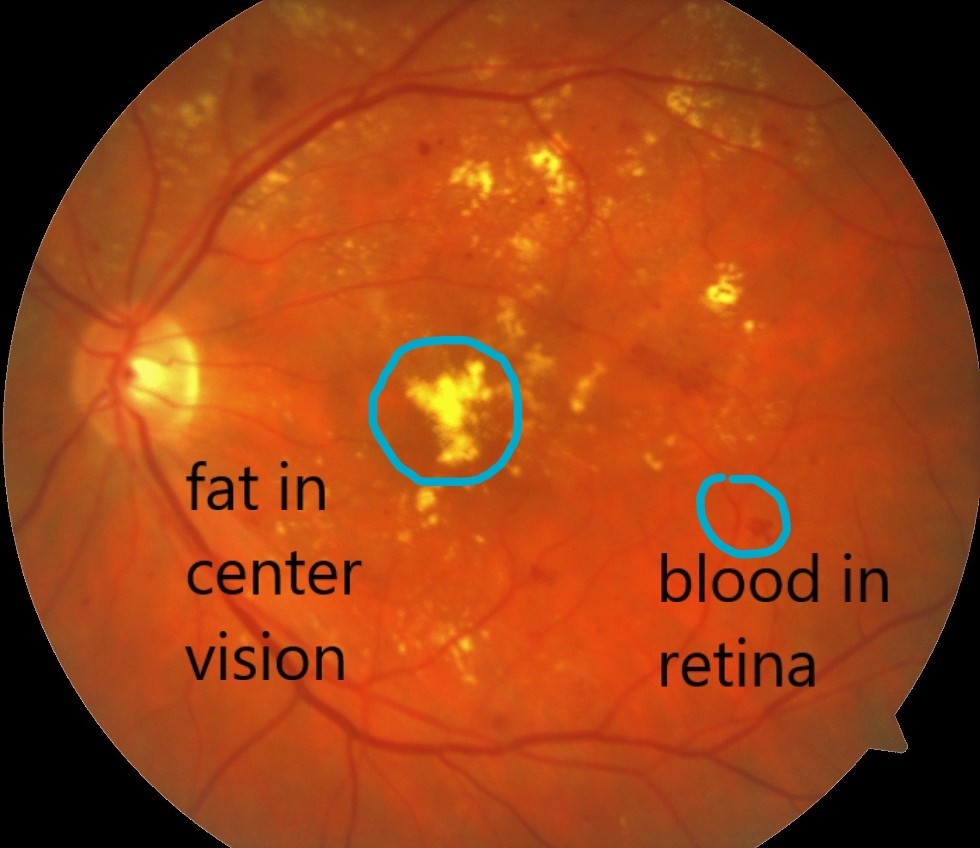
Diabetic Macular Edema
A newer treatment may be better for saving and improving vision, especially for people with diabetic macular edema, which is swelling in the center of your retina. You get shots of medicine into the jelly inside your eye. But it isn’t a cure, it’s only treatment. You’ll need to keep getting shots on regular basis. The treatment and its long-term effects are still being studied (Kozarsky, A., 2018).

3
Vitrectomy
In the late stages of diabetic retinopathy — if your retina has detached or a lot of blood has leaked into your eye — your doctor may suggest this operation to remove scar tissue, blood, and cloudy fluid from inside your eye. Vitrectomy can improve your vision (Kozarsky, A., 2018).

Who Gets Diabetic Retinopathy?
Eventually, nearly everyone with diabetes have possible chance to get iretinopathy. The longer you have the diabetes, the more likely you can det diabetic retinopathy. Your odds will be higher when you don’t have good control of your blood sugar or you have high blood pressure or cholesterol. You can also help prevent it by quiting smoking (Kozarsky, A., 2018).
3
Glaucoma
Glaucoma caused by increases peressure inside in eye. It can cause bright halos or colored rings around the lights, and it usually has no symptoms. You can lower the pressure inside your eye with drops or with laser or conventional surgery. If you don’t treat it, the pressure can damage your optic nerve, resulting in vision loss and blindness. While anyone over 40 has a greater risk, people with diabetes are 40% more likely to get it. (Kozarsky, A., 2018).


Vision with glaucoma
Cataracts
A cataract makes the lens in your eye cloudy, or milky. This blocks light, and your eyes see everything as hazy. Poor control of blood sugar can speed up this process. You’re 60% more likely to get cataracts with diabetes – and you’ll probably get them at a younger age. Surgery can replace the cloudy lens with a clear artificial one, but sometimes diabetic retinopathy gets worse afterward (Kozarsky, A., 2018).
3
See Your Doctor Immediately!

Get emergency care for any sudden vision loss immediately (including a “curtain” coming down over your vision), flashing lights, double vision, or severe eye pain or pressure. Don’t ignore these symptoms:
-Blurry or hazy vision;
-Spots, floaters, or shadows;
-Waviness or distortion of straight lines
make an appointment with your eye doctor as soon as possible (Kozarsky, A., 2018).
Protect your eyes. Get a yearly eye exam. Your doctor can look for damage or diseases.